Pelvic floor dysfunction is a common problem faced by women especially during pregnancy and post-child birth. It is however ignored as a problem that affects the performance and quality of an athlete’s life.
Athletic population is at a very high risk of developing stress urinary incontinence, both in men and women equally. It has been estimated that as many as 12.5-80% of women athletes suffer from PVD, even if they have never been pregnant or given birth.
Stress incontinence occurs in athletes due to increased pressure in the abdominal cavity resulting in urinary leakage while performing high load and high impact activities. Longer periods of increased pressure can cause extreme levels of fatigue in the pelvic muscle groups leading to leakage even during small acts of coughing and deep breathing.
Pelvic pain is commonly observed postpartum or as a result of chronic pressure caused during basketball and gymnastics. Diagnostics at NYDN are highly advanced and technological in diagnosis as well as treatment for relief from pelvic floor dysfunction and its related pain.

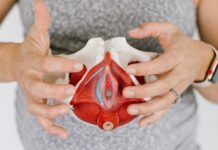
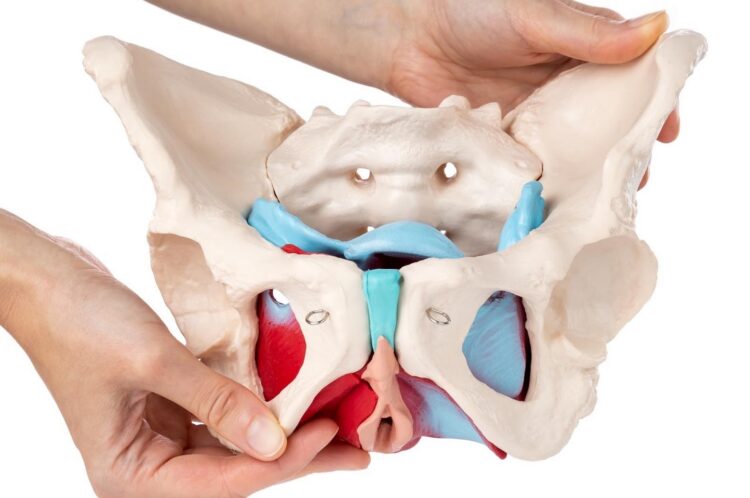
What is the pelvic floor?
The musculature supporting the area extending from the pubic bone to the coccyx comprises the pelvic floor. Superoinferiorly, it extends from obturator internus to greater trochanter. The pelvic floor muscles support the internal organs and their functioning including bladder and bowel emptying.
It also supports the reproductive organs in females.
Risk factors associated with the development of PVD
Certain factors increase your chances of developing PVD at any point of your life. Some of these factors are:
- Complicated vaginal deliveries.
- Multiple vaginal deliveries. The risk increases with every subsequent delivery.
- Twin deliveries.
- Vaginal delivery for high birth weight infants.
- Increased age of the mother at the time of conception and delivery.
- Obesity.
- Chronic constipation can damage the nerves resulting in fecal incontinence.
- Traumatic injury to the pelvic musculature.
- Radiotherapy given for prostatic cancer can reduce the muscle tone.
- Frequent indulgence in high impact exercise.
- Chronic coughing increases abdominal pressure and can lead to pelvic prolapse.

Symptoms of PVD
When the muscles and supporting tissues of pelvic floor gets impaired, you can suffer from many disorders, which are collectively referred to as pelvic floor dysfunction. The symptoms of PVD could be:
- Bowel or bladder incontinence and discomfort.
- Delayed or incomplete bladder emptying. The residual urine can cause bladder and kidney infections and can also increase your chances of developing calculi.
- Sex can become painful for some.
- Vaginal, rectal, or uterine prolapse can cause bulging or bearing down sensations during bladder and bowel movements.
- Lower back pain.
- Accidental urinary leakage while coughing, laughing, or exercising.
- Increased urinary frequency.
- Testicle or penis pain due to unexplainable causes.
- Erective dysfunction, painful and premature ejaculation in men.
- Pelvic, genital and rectal pain.
Physiology of PVD in athletes
Increased IAP (intra-abdominal pressure) is the most common cause of SUI in athletes. The 3 most common exercise modalities that result in any pelvic floor impairments are:
- Jumping
- Landing
- Valsalva maneuver
The first 2 modalities produce greater IAP antero-posteriorly for shorter duration. Valsalva on the other hand affects the pelvic floor supero-inferiorly with lesser intensity, but for a longer duration. Valsalva maneuver is commonly caused during heavy weight lifting activities.
Exercising cannot be always associated with a better tone of pelvic floor muscles as it can increase the width and stiffness of levator hiatus, which in turn increases the risk of development of PVD and organ prolapse.
Treatment of PVD
PVD can be treated with medication, surgical intervention, and physiotherapy. Normally a combination of 2 or 3 modalities is used to correct your symptoms. Medicines can be given for bladder relaxation and for reducing urinary frequency. Hormonal replacement is given in post-menopausal women suffering from the condition.
Prolapse is generally treated by implanting a surgical mesh to keep the organ in place. However, surgeries are invasive, carries a risk for infection, and might not be permanent and need subsequent procedures.
Physiotherapy can assist both the above modalities to achieve better control over the pelvic muscles. A good PEMT program can help you with exercises and even with behavioral modification necessary to adhere with the training of pelvic floor muscles for a duration long enough to provide noticeable changes.
Intra-vaginal vibratory and electrical stimulus can help in improving the strength of pelvic floor musculature in women.
Pelvic floor muscle contraction techniques
Following a right contraction technique essential to exercise these muscles and ensure a properly toned pelvic floor. There are two types of contraction techniques:
- Fast contractions are achieved by contracting and relaxing continuously. These help in activating the muscles.
- Slow contractions are achieved by contracting, holding, and relaxing the pelvic floor muscles. These are essential for building strength and endurance in the musculature.
You are supposed to do both the exercises for 10 consecutive repetitions thrice a day for a minimum of 3 months to notice any results.

Lifestyle changes for a healthier pelvic floor
You can reduce your chances of developing PVD or reducing its symptoms by including some lifestyle related changes along with treatment and exercise such as:
- Lose weight if your BMI is over 30.
- Do not indulge in heavy weight lifting and strenuous activities if you suffer from prolapse.
- Reduce fluid intake especially during later half of the day to prevent nocturia.
- Women with overactive bladder must reduce their caffeine intake to improve incontinence symptoms.
- Increase your fiber intake to ease out pressure during a bowel movement, especially if you suffer from chronic constipation or a prolapse.
Patience is the key here. PVD cannot be correct with a weakly dose of any medication or starting an exercise program. Some people notice changes early while some take more than 5 months to get any relief.
Pelvic floor health is often neglected and most people are embarrassed to discuss it with their clinicians. However, it can be easily corrected with treatment and various exercise modalities. Training yourself to engage these muscle groups during resistance activities can prevent PVD from occurring in the first place.